China’s Cabinet: Hospitals Must Accept HIV-Positive Patients
Yuan still remembers the day she took her HIV-positive son to the hospital for an epilepsy surgery. After doctors did a checkup, they tried to persuade Yuan that her son’s epilepsy was not a big deal, and tried to convince her to give up on the surgery.
“Mom, they were lying,” Yuan remembers her son — then about 10 years old — saying when they walked out the door. “They didn’t want to treat me because I’m different.”
Hospitals refusing treatment is one of the biggest problems faced by China’s roughly 800,000 people living with HIV or AIDS, many of whom have a hard time finding willing hospitals when they need surgeries.
The 13th Five-Year Plan on HIV/AIDS prevention, issued Sunday by the State Council, China’s cabinet, re-addresses the rights of people living with HIV/AIDS. It states that hospitals must not shirk their responsibilities and refuse patients with HIV/AIDS under any circumstances. But some experts say the plan will not have much of an effect if more specific measures to implement it are not also provided.
“The rule is not new to us, but it has not been implemented well over the years,” said Zhang Ke, a doctor at Beijing You’an Hospital, which specializes in treating infectious diseases, including HIV/AIDS. Government regulations issued in 2006 forbid doctors to refuse patients with HIV/AIDS, Zhang told Sixth Tone.
Many of Zhang’s patients come to You’an Hospital after being turned away by general hospitals because they are HIV-positive. Last month, on lunar new year’s eve, he received an emergency call from a friend. She told him that during preparations for an intestinal surgery, doctors had discovered her 20-year-old son was HIV-positive. The young man almost fainted in the hospital, but the doctors nevertheless insisted that they could not perform the surgery. He was eventually transferred to an infectious disease hospital in Beijing.
Such cases are regular occurrences in China, said Zhang, and the situation hasn’t changed much in recent years despite the 2006 regulations. The new Five-Year Plan does not stipulate punishments for doctors who discriminate against HIV carriers, and do not clarify under what circumstances patients can and cannot be referred to specialized hospitals for treatment. “These doctors do not need to refuse you explicitly,” Zhang said. “They can reject the patients with professional suggestions that the patients don’t have enough medical knowledge to rebut.”
The separation between general and specialized hospitals for infectious diseases has isolated patients with HIV/AIDS: While they can get treatment at the specialized hospitals, only in recent years have these hospitals begun to add surgical departments — and their capacity for such treatments is still insufficient.
After being refused by local hospitals in Zhengzhou, the capital city of China’s central Henan province, Yuan took her son to several big hospitals in Beijing. But every time she told them her son was an HIV carrier, they immediately referred her to infectious disease hospitals, which at the time did not have neurology departments.
Tired of these frustrations, Yuan saved money for years to pay for another of her son’s surgeries in Hong Kong, this one costing her more than 100,000 yuan ($14,500). “The city we live in has the world’s biggest hospital, yet we have to travel all the way to Hong Kong,” she said.
Despite advocacy groups trying to bring attention to the plight of people living with HIV or AIDS, these individuals still face discrimination in many facets of daily life. Children are ostracized by their neighbors or parents of classmates; a survey published in late 2016 showed that most women who are HIV-positive are victims of domestic violence; and in Guangzhou, a megacity in southern China, a 27-year-old man has been fighting a legal battle for months because he lost his job after his employer found out he was HIV-positive.
Discrimination and misconceptions are stubborn and hard to fight, in part because many Chinese people living with HIV/AIDS fear that revealing their carrier status will mean dismissal from their job. The five-year plan — again echoing existing regulations — says that the right of people with HIV/AIDS to work should be protected but does not elaborate on the precise form that protection should take.
Zhang believes that doctors, at least, should know better. “The risk of transmission from patients to doctors during surgeries is low, at about 0.03 percent,” he said, adding that post-exposure prophylaxis can prevent HIV infection and is free in China for people in relevant occupations. “I don’t understand why Chinese doctors are so scared of the word ‘AIDS,’” he said.
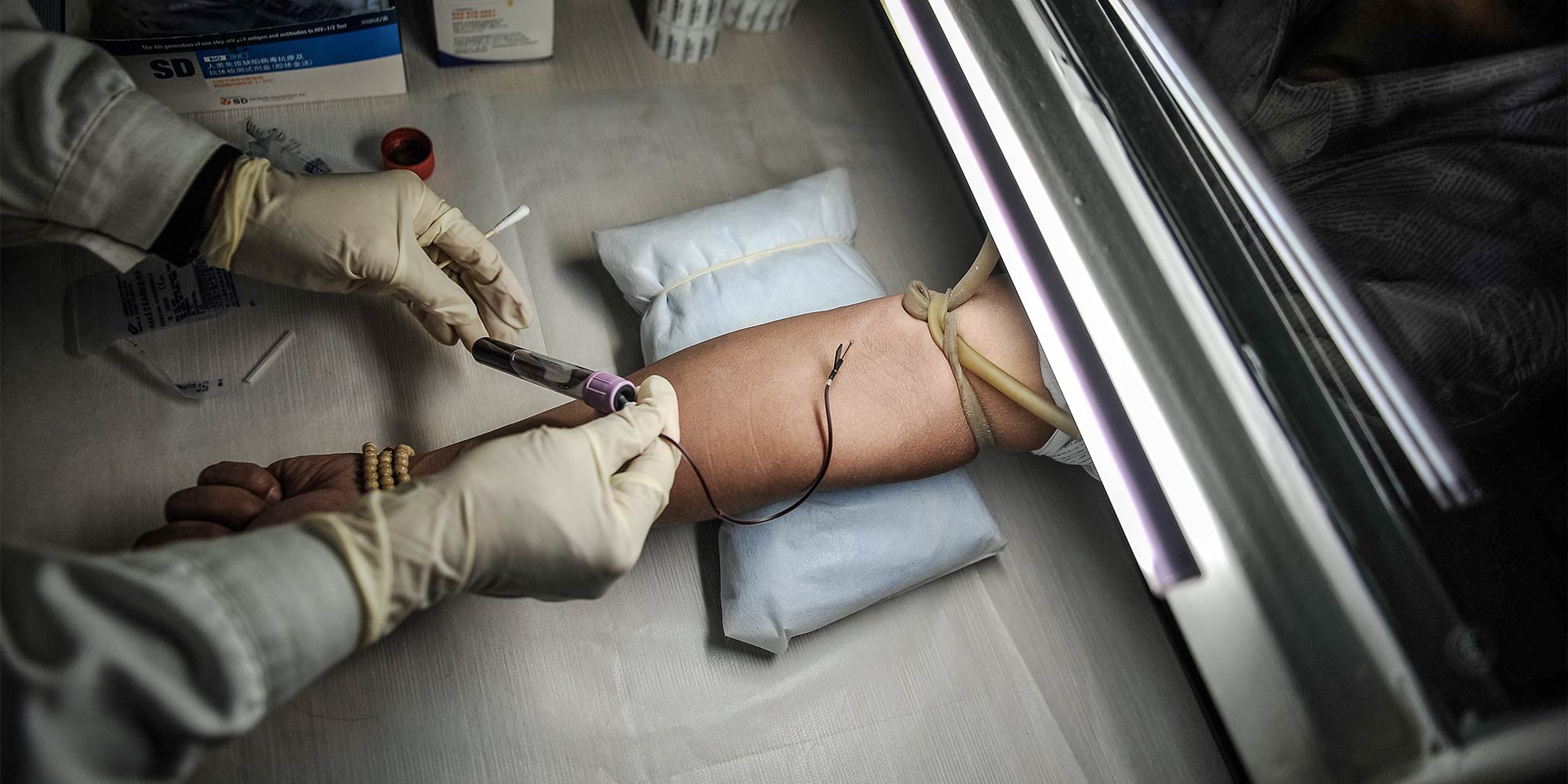
(Header image: A medical worker draws a patient’s blood to test for HIV, Tianjin, Nov. 23, 2016. You Sixing/VCG)










