China’s Palliative Care System Gives Little Comfort to the Dying
In 1960, the average life expectancy in China was just 43.4 years. By 2015, that figure had risen to 76 years. Advances in medicine and public health provision have played an enormous role in this transformation.
As Chinese people are living longer, healthier lives, they are increasingly focusing on quality of life as well. As a result, the country’s health care industry is pivoting away from a narrow focus on the provision of medicines and toward a holistic approach that serves our biological, psychological, and social needs.
More and more Chinese medical professionals are recognizing that longstanding ways of treating the sick — whereby medicines are prescribed to cure a specific ailment — view patients and disease as two distinct entities. Yet patients have needs beyond swallowing pills, attending physiotherapy appointments, or undergoing operations. They also seek psychological and emotional comfort in times of great suffering and distress.
The rapid development and deployment of medical sciences in China has led to a popular misconception in the country that medicine is an omnipotent and certain science. But in reality, medicine relies heavily on probability, educated guesswork, and compromise. Even today, we lack sufficient understanding of many diseases. Most diseases are not yet fully curable, and in many cases, we can only slow their progression.
This is the backdrop to a growing focus among the Chinese medical community on palliative care. In order to improve the quality of life of a patient and their relatives, palliative care employs many forms of intervention to prevent, relieve, and manage chronic symptoms. It is an approach to care that addresses the person as a whole, not just their disease.
Most Chinese people know little about palliative care. The Quality of Death Index, a measure of palliative care quality in 80 countries around the world released by The Economist Intelligence Unit, compares the supply of palliative care with the demand for it. While the top of the list is dominated by wealthy Western countries with strong public health systems, the 2015 index ranked China 71st for overall quality of death and 69th for its palliative and health care environment. It also showed that terminally ill patients in China are unlikely to receive palliative care. Those who do are likely to be city dwellers, as the majority of Chinese hospices are concentrated in urban areas.
The country also lacks fully equipped palliative care units. Most hospices suffer from shortages of psychologists, social workers, and volunteers. Our medical schools rarely teach palliative care to students, and there are few specialized accreditations in China that cover end-of-life care.
According to a 2016 report by the Party mouthpiece People’s Daily, China is now home to more than 200 million people over 60 years old, and chronic diseases like cancer are the primary cause of death. Yet across the country, fewer than 150 health care institutions, nursing homes, and social organizations specialize in end-of-life care, and most of those that do are community health care providers, not large-scale public hospitals.
One reason for the dearth of palliative care services is the partial modernization of China’s health service. However, socio-cultural factors also contribute to the problem. Traditionally, death is a serious taboo in China, and most people rarely speak about it. At the same time, people tend to believe — however abstractly — that life is inherently better than death, and it is therefore better to live one more day instead of giving up the ghost prematurely.
Social taboos lead many Chinese to dismiss palliative care out of hand, saying it is no different from abandoning the exact, omnipotent science of quality medical treatment. Instead of fighting to get better, they say, palliative care embraces the slow wait for death. Engrained values of filial piety and reverence for our elders mean that if an elderly relative falls seriously ill and their family members do not attempt to help them recover, then the family have failed to do their duty.
As a lecturer in bioethics, many people ask me if palliative treatments cause the patient to die more quickly. Others ask if it is the same as euthanasia, or confuse it with concepts like the right to a “dignified death.”
I tell these people that, first of all, palliative care does not speed up death. Neither does it include euthanasia or physician-assisted suicide, both of which are illegal in China. In addition, Chinese patients who say they wish to pursue euthanasia often do so because their current treatments — which are designed to prolong life at all costs — do a bad job of managing their pain and suffering. Others fear becoming a burden on their families, or wish that their nearest and dearest could better keep them company. Good palliative care targets these problems, leading some patients away from thoughts of euthanasia or suicide.
Palliative care does not accelerate death, but neither does it delay death. It provides holistic care aimed at addressing the suffering of a patient and their loved ones. This suffering might include physical discomfort like pain, digestive issues, or breathing problems. But just as importantly, it treats psychological symptoms such as anxiety, depression, insomnia, and lethargy. Patients receiving palliative care are still able to accept medical intervention aimed at prolonging their lives, but they can also choose to reject such treatments.
Finally, palliative care is a different debate from “dying with dignity.” In China, some people trying to advance the cause of palliative care use this expression to refer to terminally ill patients who die “peacefully,” having refrained from using artificial resuscitation or invasive intervention. But this usage is something of a misnomer, because “dignity” means different things to different people. If medical professionals come to equate a dignified death with refusing resuscitation or invasive surgery, for example, then we implicitly pass judgement on people who do opt for these methods at the end of their lives, who do see such last-ditch attempts as a gracious way to bow out. We hint that those who choose proactive forms of prolonging life have less dignity than those who accept death, when true palliative care respects the choices of those who go down fighting, determined to stay alive for as long as they can.
As palliative care services develop in China, we must make sure not to strip patients of their autonomy. That is the reason that living wills — also known colloquially as advance decisions — are often recommended for those who choose end-of-life care. These concepts seek to improve quality of life and help both patients and their families prepare for death. In China, these views are decidedly liberal, and it will take time before the country is ready to cast off its antiquated beliefs — for example, demanding that doctors do not inform the patient about the severity of their condition, in the misguided belief that this saves the afflicted from additional distress.
Fortunately, the situation is changing. A survey conducted last year asked 1,084 Chinese patients and their relatives in China about their attitudes toward end-of-life care. Ninety-two percent of respondents said they would want to know the truth about their medical situation and make health care decisions on their own, without their relatives’ input. Forty-four percent would opt out of resuscitation in their last moments, while 40 percent would opt out of any life-prolonging medical treatment should they enter an irreversible state of near-death.
Once we learn to truly respect patients’ wishes, we can popularize palliative care and raise the quality of life for patients and their loved ones. China’s end-of-life services should also be better regulated: Other countries say that a dying person should have access to palliative care anywhere from three months to a year before their estimated time of death. China should have its own standards and consider either absorbing palliative care into the welfare state or working it into existing forms of health care insurance.
Above all, China needs more professionals specializing in palliative care — not only doctors and nurses, but also social workers, musicians, psychologists — people trained to help others connect with the things that make life enjoyable. Death comes for us all eventually, and when it does, we can at least ensure that it is not shrouded in confusion, conflict, and fear.
Translator: Owen Churchill; editors: Zhang Bo and Matthew Walsh.
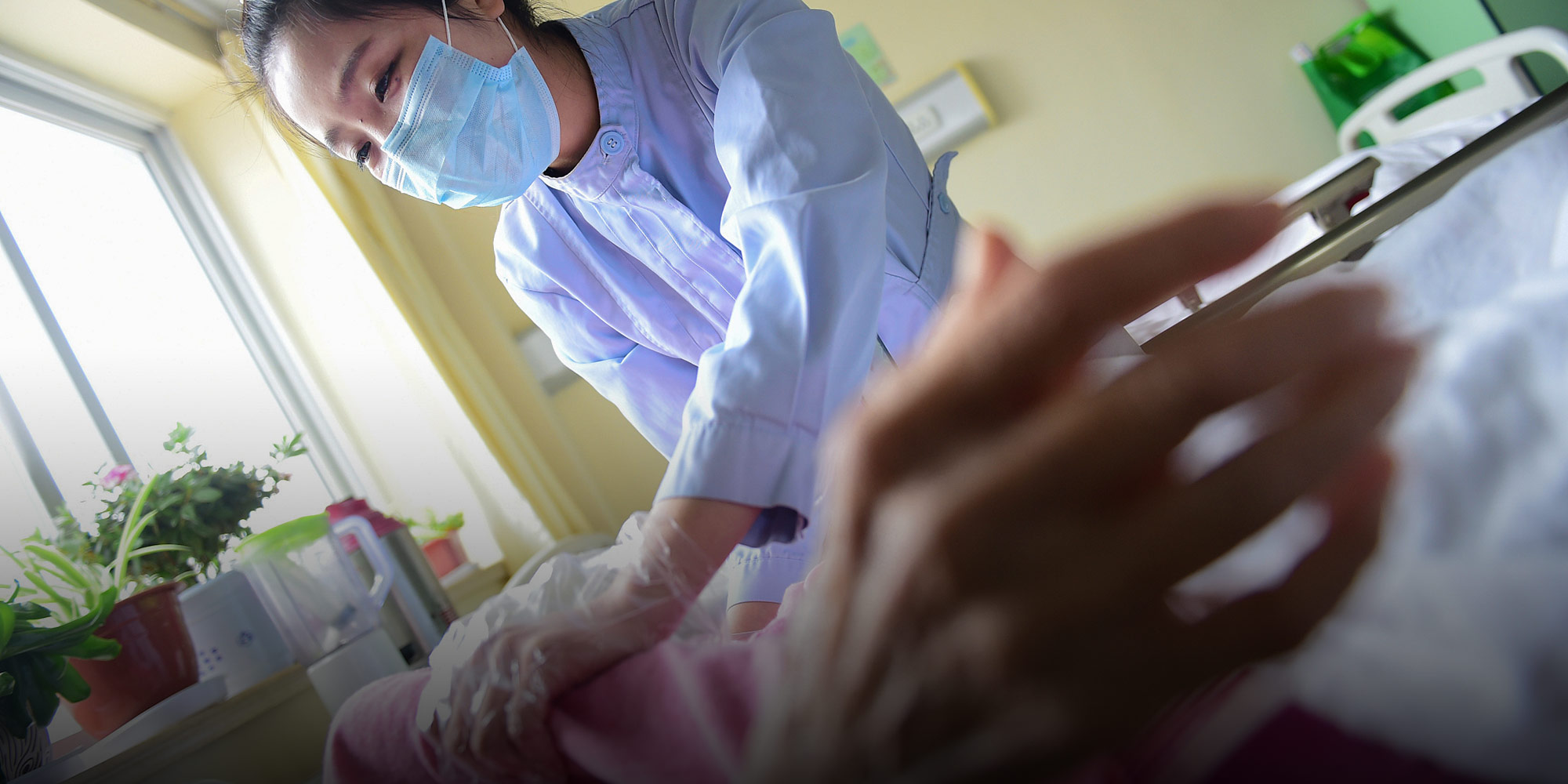
(Header image: A nurse takes care of an elderly man at a sickroom in Qingdao, Shandong province, April 20, 2018. VCG)










